 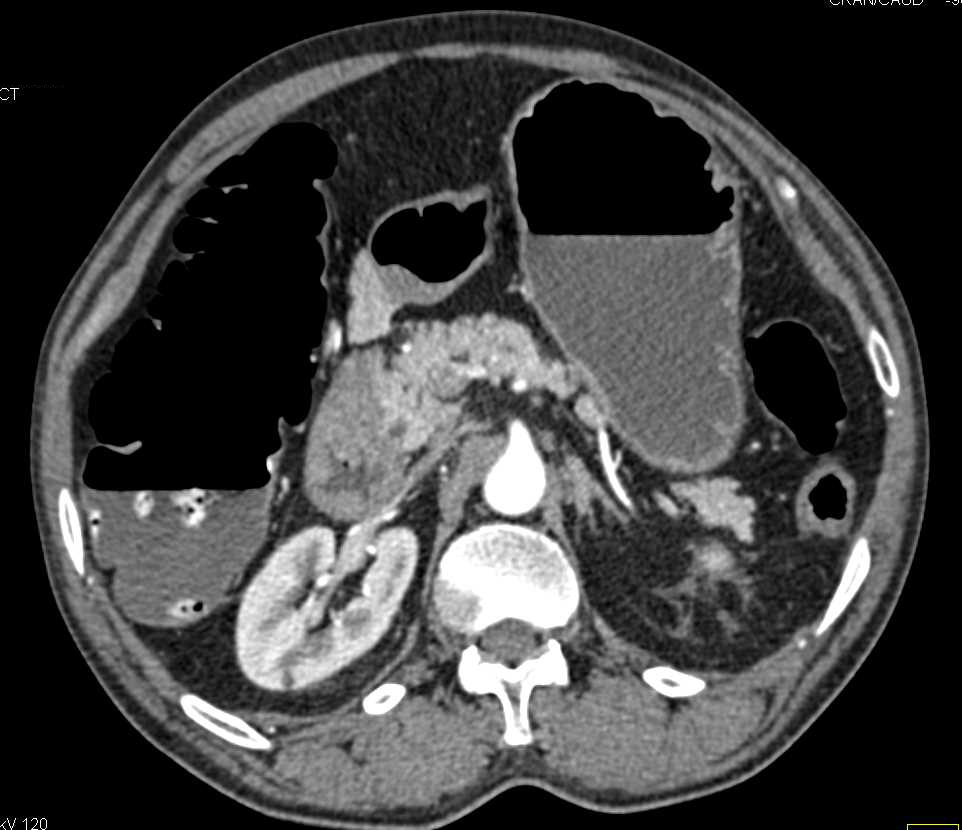 
However, a more recent French intergroup survey showed that the preferred procedure was SFC (70%), followed by LHC (17%) and STC (13%) ( 17). One anonymous practice survey of members of the Association of Coloproctology of Great Britain and Ireland (ACPGBI) indicated that ERHC is preferred by 63% of respondents, followed by LHC (23%) and SFC (14%) ( 16). Moreover, the choice of operation is dependent on several factors, including the surgeon’s preference. Some surgeons have also recommended extended resection of the spleen and distal pancreas ( 3, 13), although the benefit of this approach is under debate ( 14, 15). In contrast, other authors reported that limited resection is sufficient and that results did not indicate a survival disadvantage ( 5, 12). Some authors believe that extended resection better guarantees the removal of all potentially included lymph nodes along the superior mesenteric vessels ( 2, 10, 11). In an updated meta-analysis ( 9), a study concluded that the procedures include splenic flexure colectomy (SFC), left hemicolectomy (LHC), extended right hemicolectomy (ERHC) and subtotal colectomy (STC). Confusing nomenclature is often found in the literature ( 8). There is also some confusion regarding the definition of operations for splenic flexure cancer. Various extents of resection have been proposed, from extended procedures to segmental resection. Lymphatic drainage is variable and incompletely understood in the splenic flexure. No consensus has been reached regarding the optimal extent of radical surgery for splenic colon cancer. However, many studies have found no difference in survival compared to that of other colon cancers ( 4, 7). According to reports, splenic flexure cancer is associated with a poor prognosis due to a high risk of obstruction and diagnosis an advantage stage ( 2, 6). Splenic flexure cancer is relatively rare, representing only 2-8% of all colon cancers ( 4, 5). Cancer of the splenic flexure is defined as colon cancer situated between the distal third of the transverse colon and the proximal descending colon within 10 cm of the flexure ( 2, 3). The rate of metastatic lymph nodes at the root of the central artery and gastroepiploic arcade node was relatively low.Ĭolorectal cancer (CRC) is one of the most common gastrointestinal malignancies ( 1). Looking at long-term prognosis, no differences were observed among the three groups regarding both 5-year overall survival (94.0% vs 90.2% vs 94.1%) and disease-free survival (88.2% vs 90.2% vs 83.0%).Ĭonclusion: Our retrospective review suggests that splenic flexure colectomy in minimally invasive surgery is a safe and effective treatment option for splenic flexure colon cancer. 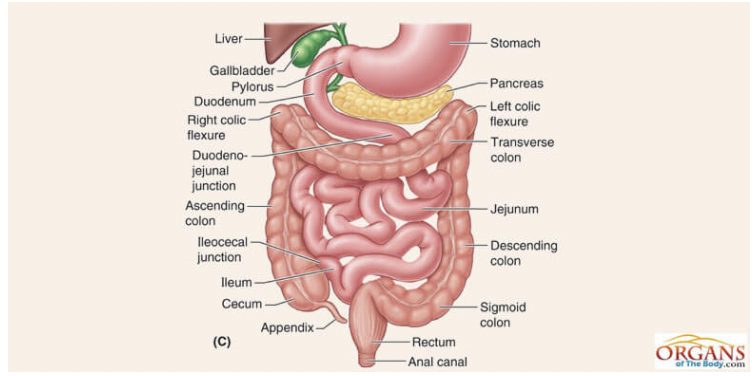
No metastatic lymph nodes at the root of the inferior mesenteric artery (IMA) were observed lymph node metastasis appeared at the root of the middle colic artery (MCA), but in a low proportion of cases (4.4%). No statistically significant differences were found among the groups regarding postoperative complications, pathological data or recurrence. We retrospectively compared the postoperative, pathological and long-term outcomes of patients with splenic flexure cancer. Methods: Between January 2011 and December 2018, 117 patients with splenic flexure cancer were enrolled in the study.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
